A Picture is Worth a Thousand Words...

Epilepsy News From: Wednesday, January 28, 2015
Why imaging is so important in the evaluation of epilepsy
For any person with epilepsy, it is important to have appropriate images of the brain to assist in determining the cause of epilepsy, expected course of epilepsy, and treatment options. Oftentimes, when someone comes to the emergency department (ED), a CT scan is performed. CT scans are advantageous because they are readily available in nearly all emergency departments, only take a couple of minutes to complete, and show any large or immediately dangerous abnormalities. However, CT scans lack the level of detail needed for a comprehensive evaluation of epilepsy. CT will detect only about 30% of abnormalities that result in epilepsy.
Magnetic resonance imaging (MRI) allows for detailed imaging of the brain and visualization of subtle or small abnormalities that may result in epilepsy. MRI allows for identification for causes of epilepsy such as medial temporal sclerosis, malformations of cortical development, and low grade or benign tumors. All of these findings can result in long term epilepsy – emphasizing the need for imaging – even in someone with a long history of epilepsy! Once it is known which area of the brain seizures arise from, extra review is often required. With extra attention to a specific region, subtle lesions can sometimes be found that were missed in the initial review.
Example 1
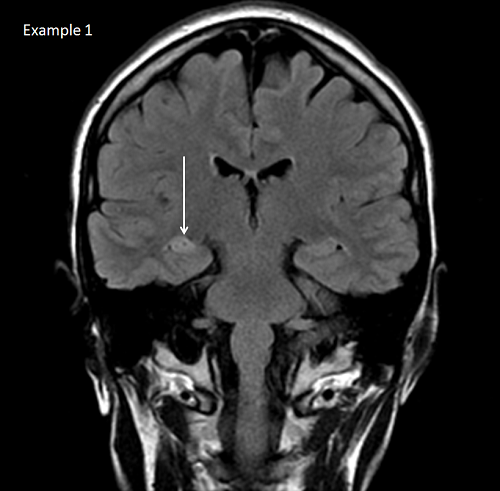
This MRI is from a 36-year-old woman with an 8-year history of epilepsy. Her first seizure was a generalized tonic-clinic seizure. She continued to have complex partial seizures, which were not controlled despite trials of multiple medications. A repeat MRI was performed, and right mesial temporal sclerosis (MTS) was seen. MTS is the most common cause of epilepsy that is refractory to medical therapy. In these cases, surgery offers the greatest chance of a cure for epilepsy.
Example 2
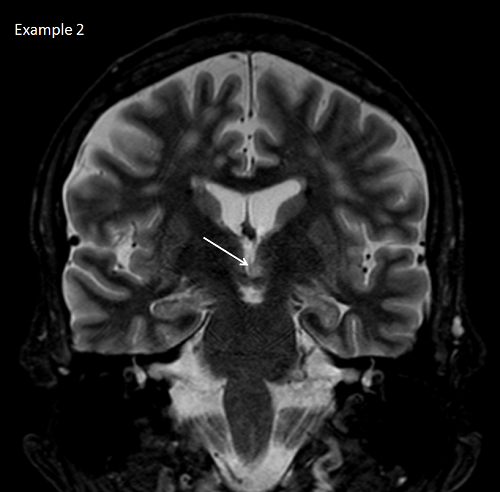
This MRI is from a gentleman that was referred for spells. He describes a lifelong history of recurrent "laughing" spells, without loss of awareness. His wife states she can tell when he is having the events, because he will have a brief smile, which is not his normal smile. He had at least one CT in the past, which was normal, but never an MRI. The arrow points to a hypothalamic hamartoma. These are noncancerous growths in the hypothalamus that characteristically cause laughing or "gelastic" seizures. Other seizure types can occur, including generalized tonic clinic seizures. Treatment options include surgical resection, focused radiation, or laser ablation.
Authored by
Amy Z. Crepeau MD
Reviewed Date
Wednesday, January 28, 2015
